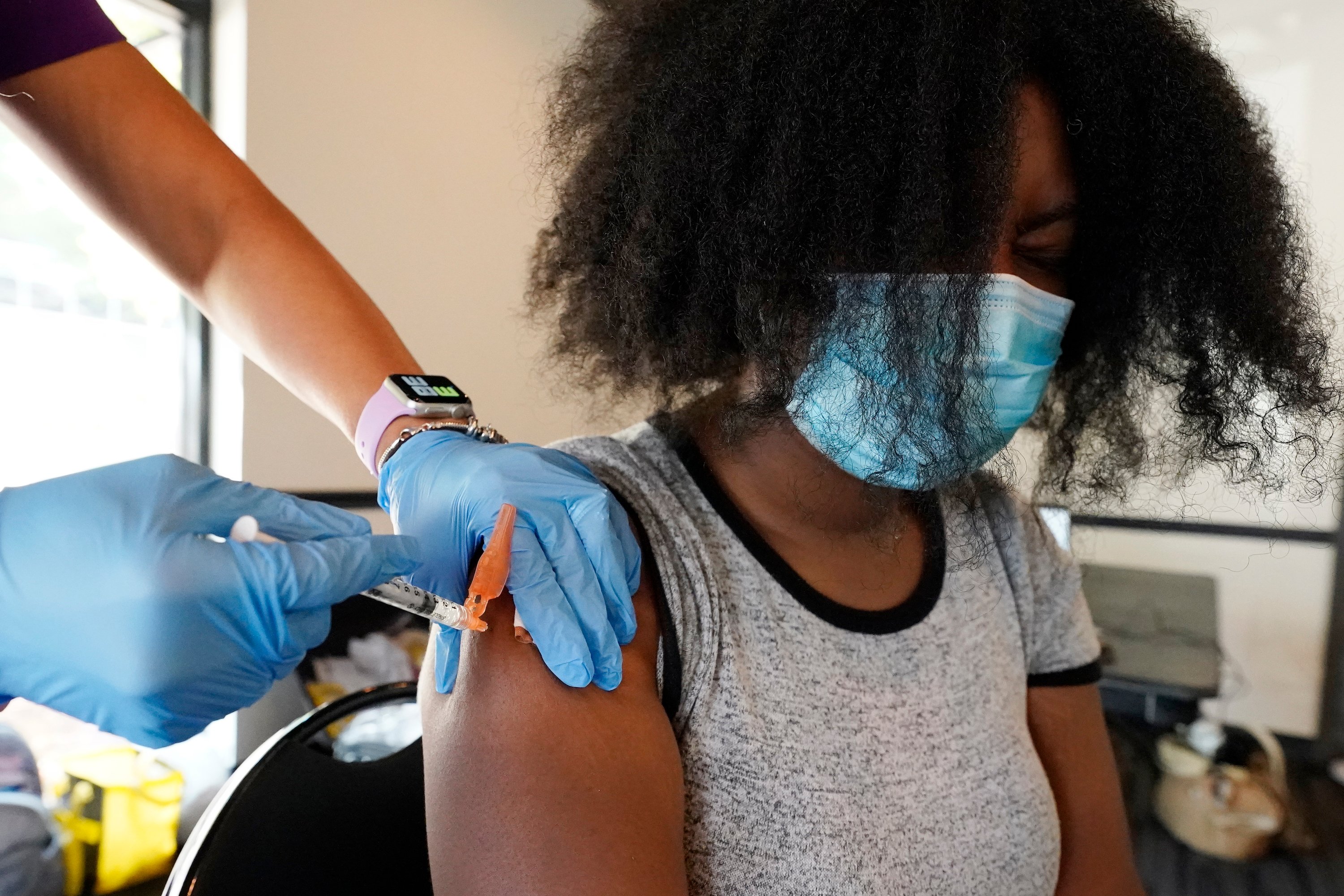
My body was taken over by unbearable aches and chills. I cried my eyes out to a registered nurse in the emergency room where I had been waiting for over five hours. She looked at me unconcerned, ready to pass me off to the next available person. Barely able to speak through the tears, I told her and another nurse that I was experiencing excruciating pain from head to toe. I remember telling them that my pain was “beyond a 10.”
Yet I was sent back to the waiting room for an additional two hours.
Nothing was done to help with the pain—not even a hypothesis of what could possibly be wrong. I waited, shivering and in agony, before I was taken back to have blood drawn and a CT scan. It was in that moment I realized they were just checking boxes. It didn’t matter that I was pleading with the nurses about the excruciating pain. They were just trying to push me along.
Another hour passed before I was called to the back again. The results of my blood tests and CT scan didn’t reveal anything. They told me I “probably just had early symptoms of the flu,” but they didn’t give me a flu test. I was sent home with a 500mg prescription of Aleve. After nearly seven hours in that emergency room, all I received was a “probably.”
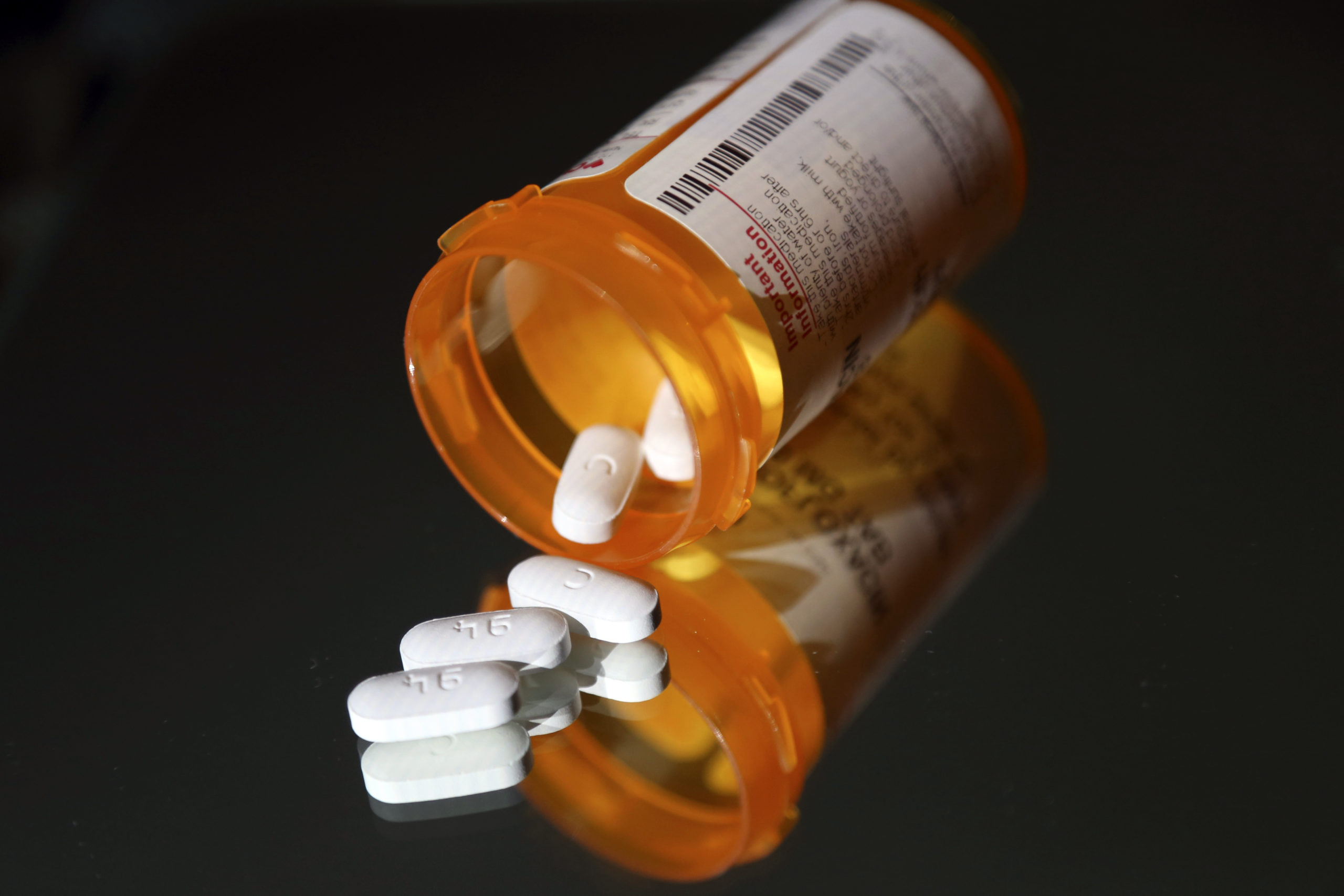
The pain persisted for two and a half weeks more. Luckily, I am here today, along with others, to tell my story.
America’s healthcare system fails Black women time and time again. Living in a first-world country with such stark health disparities for Black women is not only infuriating but disheartening. So, where did this implicit bias and racial inequality in our healthcare system come from?
Take it back to the 19th century and a well-known surgeon by the name of J. Marion Sims. He is considered the “father of gynecology,” but he is rarely criticized for his controversial approach to medicine. He believed that Black women could not feel pain, so he developed his techniques by operating on enslaved Black women without anesthesia. While the execution may be less crass, the problem persists today—healthcare professionals are not listening to us or believing our pain!
I spoke with Tierney Dean, 23, who was diagnosed with idiopathic intracranial hypertension. To put it plainly, she was experiencing severe, crippling headaches because of pressure on her brain. Had this condition gone untreated, she could have lost her vision.
“I had headaches where I would have to stop in my tracks,” she explained. “I couldn’t function, so I knew something was wrong with me.” Tierney’s mother, to whom she’d expressed her pain several times, took her daughter to see multiple doctors over the span of 10 visits. “Every time they would say, ‘You must not be drinking enough water. This must just be a migraine,’ and so on. But I kept telling them this wasn’t just a regular migraine or headache. They made me feel crazy.”
Along with Tylenol and other medications for migraines, Tierney was also prescribed anxiety medication, as her health anxiety skyrocketed because she knew in her heart something was wrong. Then, during a visit to her optometrist—a Black man, a routine eye exam and some imaging revealed that there was swelling behind her eyes.
“When he did my eye exam,” said Tierney, “and I was telling him how I felt, he was like, ‘The images came back, and it looks like there’s swelling behind your eyes. That could mean two things: either you’re taking too much medication and it’s building up behind your eyes, or you have a brain tumor, so I need you to go to the hospital right now.’”
Emotional, she followed his orders and rushed to the hospital, outlining to them all that the optometrist told her she needed. Her cry fell on deaf ears once again. “When we got to the hospital,” she said, “the doctors there told me it wasn’t severe enough for an MRI.” They prescribed her more medicine for the headache and recommended she drink more water before sending her home.
Luckily, Tierney was able to book an MRI at a private imaging center. “From there,” she said, “everyone started taking me more seriously.” She was referred to a neuro-ophthalmologist who was able to diagnose and treat her.
Sadly enough, our cries as Black women don’t stop there—they echo throughout the daunting and precarious journey into motherhood.
Madison Simon, 22, went to the emergency room in excruciating pain. She was 11 weeks pregnant at the time and just days away from her second trimester. She pleaded with nurses to check on her baby. “They told me if I see bleeding,” said Madison, “I need to call my OB[GYN].” After prescribing her some Tylenol and discharging her, she miscarried the same day at home. “It felt like their mindset was ‘how many can I get in and get out?’” Madison said. “It felt like a business, not like they genuinely care about the patient or their well-being.”
If she could speak to the doctors and nurses today, what would she say? “I just wish you all would have checked for my baby’s heartbeat…” says Madison. “To have experienced that after just leaving the hospital—I was traumatized.”
According to Black Women’s Health Imperative, when it comes to Black women and motherhood, we are three-to-four times more likely to die from pregnancy than our white counterparts, and we experience the highest infertility rates. According to the Centers for Disease Control and Prevention, “In 2021, the maternal mortality rate for non-Hispanic Black (subsequently, Black) women was 69.9 deaths per 100,000 live births, 2.6 times the rate for non-Hispanic White (subsequently, White) women. Rates for Black women were significantly higher than rates for White and Hispanic women.”
These traumatic experiences of implicit bias prevent Black women from getting the care they deserve.
Sydney Eason, 25, recalls the almost horrific experience of her mom giving birth to her youngest brother, Nick. While sitting in the living room watching a movie, her mom started feeling some discomfort. The pain grew more severe, and everyone urged her to go to the hospital.
“I remember being in the hospital room with my mom,” Sydney explained, “and she was explaining to them over and over that something didn’t feel right. This went on for at least two hours. My dad was getting frustrated, and the doctor threatened to remove him. I remember this like it was yesterday—the doctor told my dad, ‘Your wife isn’t the only woman having a baby today. The nurse said she’s fine. I don’t want to have security remove you.’”
Moments after sitting there, they heard Nick’s heartbeat, which sounded irregular. Shortly after, they heard the line go completely flat. “Nick’s umbilical cord was wrapped around his neck for 45 minutes,” Sydney recalled, “and [it] was getting tighter the more he moved. My mom had to have an emergency C-section.” From that moment she developed a distrust with healthcare providers. To this day, Sydney despises going to hospitals.
And she’s not alone. These stories here barely scratch the surface and should serve as more than enough explanation for why we don’t feel safe in the hands of those meant to strive to protect our well-being.
The neglect of and bias against Black women is a danger to us all, and I hope that through this piece, I not only gave a voice to the voiceless, but I’ve also urged all Black women: when you are put in that situation, make them hear your cry—do not give up.